Rehab after stroke
A personal story about rediscovering my left arm and hand
Some background
Eight weeks ago (24 September) I had a stroke.
I’m really lucky:
- many people have worse strokes than I did (I kept my cognitive abilities and understanding of language, I didn’t have any memory loss, I don’t have any vision problems, I can walk, I’ve not had not any pain, my speech was only slightly impaired; the key impact for me was that I was paralysed in my left arm — and I’m right handed), and
- I’m making a good recovery (probably helped by being relatively young, I’m 44).
People say that no two strokes are the same.
I would add that no two stroke recoveries are the same either.
In a blogpost about my stroke that I published two weeks after I’d had it, I compared recovering from a stroke to climbing a mountain — a daunting prospect and something that is best done slowly, by taking small steps. I then wrote about many aspects of my recovery (sleep, trying things, walking, and some of the emotional complexity I’ve been experiencing) in a separate post.
The main focus for my recovery is physical rehab for my left arm and hand, which at first were completely paralysed, and that’s the subject of this post.
Neural connections, muscles, body maps, and space
Small bits of spontaneous recovery started for me within 24 hours, with fractions of isolated movements returning to my shoulder and upper arm. This could happen at any time, often over night. For example, one night in hospital I felt my left bicep randomly start to fire and twitch: a good sign, my brain was beginning to re-establish a connection to the muscle. Most of the time, once there I kept this new neural connection. Occasionally, I lost it (and the associated movement) and had to get it back again later.
This sort of spontaneous recovery reveals one of the weird things about paralysis of a limb immediately after stroke: the reason you can’t move isn’t because you’ve suddenly lost your muscles, they haven’t wasted away overnight; the loss of mobility is caused by brain damage rather than damage to the muscles. Over time, things move on: my left forearm is now thinner than my right forearm, and that’s because I haven’t been using those muscles, so now it is a question of needing to build up muscle strength in my arm, as well as the strength of the necessary neural connections for those muscles.
It’s scary how easy it has been for me to forget my left arm and to do everything one handed (particularly as I’m right handed). Occasionally it’s that I deliberately don’t bother to include my left arm/hand in what I’m doing (as involving it can slow me down); much more often, I simply forget about it. It’s like my brain is ignoring my affected arm or has momentarily cut it off, and I often have to remind myself to involve it, or Rebecca, my wife, reminds me.
It’s so easy to lose musculature and neural connections this way, that it’s got a name: ‘learned non use’. When someone who has had a stroke tries to use their paralyzed arm and finds that they can’t, they ‘learn’ not to use it and rely on their functioning arm instead. Brain expert Norman Doidge explains that the result is that, “not being used at all, the circuits in the brain that govern the paralysed arm waste away,” It can be a vicious circle caused by the brain being a “use it or lose it organ”. Because it’s plastic, the efficient brain will either shut down those unused connections or repurpose them for something else more useful.
So the first thing is to find or make neural connections for my affected arm/hand (this is possible thanks to the brain’s neuroplastic ability to change its own neural networks by adding new cells or by creating or repurposing nearby connections to take over the connections I lost in the area damaged by my stroke), and then I need to keep using them, building up my familiarity with the movement and the strength of the muscles.
This is hard.
At first, when I’m trying to find a connection between my brain and the finger/wrist/portion of my affected arm that I’m trying to move, I find little or nothing there, and so my brain tries other neural connections. One consequence is that, in order to move a finger on my affected left hand, I might also move the corresponding finger in my right hand, or my left foot, or my left thigh, my abdomen, my left shoulder, or my neck. I imagine it looks by turns comical or strange to see me straining other body parts in order to move a finger just one millimetre. I don’t really care. I’m so focused on regaining my movement it doesn’t bother me too much how I look. As Tom Balchin puts it in The Successful stroke survivor, a tiny movement opens “a world of potential”. The joy of (re)discovering a movement in my hand/arm is so great that the rest doesn’t matter. If in order to make that neural connection, I also fire off other muscles, so be it. The key thing for me is to find that initial connection, to remember again how it feels to make that movement (perhaps it’s about creating ‘muscle memory’ — the real ‘memory’ resides in our brain, of course). Once I’ve rediscovered that neural pathway, I figure that over time I can work on improving the quality of the movement and gradually filter out the other messages that my brain is also firing to other muscles at the same time.
Another impact of me not using/moving my left arm is that without movement we lose awareness of our body in space. My mental image of my body (we each hold a ‘map’ of our body in our brain) begins to change and sometimes it no longer includes my affected arm. Consequently, as I move through space I take no account of it, meaning that I would sometimes bump into doorframes on my left-hand side as I walked through them. (Other examples of my mental ‘body map’ being ‘off’ include my left hand banging into my left thigh when I walk, rather than swinging past it, and my left hand hitting the back of my head when I lower it after having held my extended arm straight up above my head.) Overtime, I redraw my mental body map to once again include my arm (and in the correct relation to the rest of my body). This is helped by me slowly coming to comprehend and appreciate — thanks to Rolfing and Feldenkrais — that, unlike the image I have of an action man doll, my arm is not actually a separate body part, easily distinguishable/ separable from my torso (and nor is my hand separate from my arm); there are a huge number of ways that the arm connects with the body, through muscles and fascia, just as muscles that move your fingers are in your forearm.
My shoulder and gravity
My recovery follows the classic pattern for an upper limb after stroke: movement comes back from the trunk towards the hand. That is, I regain the ability to move muscles around the shoulder before those in the upper arm, which comes before my lower arm, and moving my fingers comes last.
Rehabilitating my shoulder is relatively straight forward. However, I get a shock when I see a photo of my shoulder, because it looks like my left shoulder blade has disappeared:
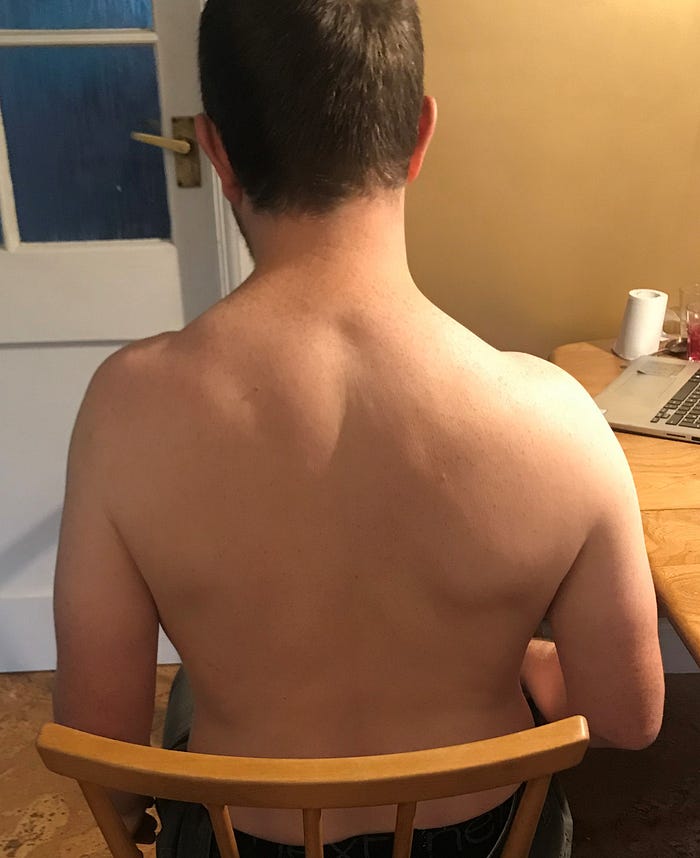
In reality, it’s a combination of two things: first, I’m not properly firing my left rhomboid muscle (your rhomboids are in your upper back and connect the inner edges of your shoulder blades to your spine; I find it difficult to visualise my rhomboids) and I’ve been over-compensating by using muscles at the top of my left shoulder instead to do the work of the rhomboid; and second, my left shoulder has been pulled round by the weight of my left arm. I had no idea how heavy my arm is and had some how failed to appreciate what a powerful force gravity is. Normally you hold the weight of your own arm without thinking of it, but when I can’t do that any more, I suddenly realise how much it weighs. Moreover, gravity really pulls it down (and my shoulder with it), and learning to lift my arm again against gravity is going to take some doing. The physio is not too concerned though, and he gives me some exercises for my left rhomboid, which he gradually makes more demanding as the weeks pass. Also, for the first couple of weeks, I wear a collar and cuff sling whenever I walk to support the weight of my arm and take the load off my shoulder. This not only helps my shoulder; it also helps my walking, as the weight of my arm was affecting my posture.
My arm
Rehabilitating my arm is relatively uncomplicated too. Over the weeks, I gradually and naturally relearn how to do the various movements, and only one issue requires more focused rehab. My left tricep (or my mental connection to it) is particularly weak — more so it seems than some of my other arm muscles — and this goes along with my bicep rarely extending to its full length, so consequently the bicep muscle shortens, making it a double effort to fully straighten my left arm. For weeks I cannot put any weight through my arm without my elbow flaring out. Again though, the physio is not too concerned, and he gives me some exercises.

Adding in weight
I gradually progress from not being able to move my arm, to being able to lift my whole arm, or just my forearm, or just my wrist. I then progress to being able to hold my arm up against gravity in an elevated position for a couple of seconds, or to doing five and later ten repetitions of an exercise. After about six weeks I progress from there to being able to lift a small weight — a child’s wooden brick first and then on to lifting a kilogram, which is exhausting, and I need to go for a lie-down afterwards.

Tom Balchin, who has trained over a thousand stroke survivors as well as professional trainers & therapists, is clear on the need for physical rehab after a stroke to follow a progressive training program that includes bodyweight exercises and weight training, always training at a sufficient intensity level to enable physiological adaptation to occur. As he explains in The Successful stroke survivor, “muscle growth and the strengthening of tendons and ligaments does not occur by accident.” They can only grow stronger through resistance training, where the body “adapts to the stress of training, then overcompensates just a little to cope with the next time.”
The more I recover, the more I discover that I can’t yet do
At first, the issue with my affected arm feels relatively simple — there’s just one thing I can’t do: move my arm. As my rehab progresses, I discover more and more things that I can’t do with my arm in the way that I used to: moving it like this or rotating it like that, and this experience is repeated and multiplied for each individual part of the limb (lower arm/wrist/hand/ finger/knuckle).
It is like discovering that my route up this recovery mountain passes along many peaks: when you’re climbing towards the first peak on your journey, you can only see one peak and so you might think that you’re getting to the top of the mountain, but once you’ve scaled that peak, other peaks beyond it are revealed for the first time and you understand that the real summit is both further away and higher than you had previously realised.

In some ways, physiotherapy feels like a cruel discipline. It precisely pinpoints what you can’t currently do and give you exercises related to that inability. Every new exercise brings home to me a movement that I can’t yet do and asks me to repeatedly spend energy and time on it.
Tom Balchin’s fantastic book The Successful stroke survivor contains over 150 pages of exercises for the upper limb. And I get others from my physio. Yet again, I’m thankful that I don’t have to rehabilitate my leg as well.
I compare re-learning to move my arm/wrist/hand/fingers to when we first learn these movements and I think how long a baby spends practicising these movements over and over again.
My hand
The hardest aspect of my physical rehab is my hand. This is normal for stroke survivors: it’s the most complicated part of the upper limb, with an amazing number of bones and soft tissue connections and a correspondingly amazing range of subtle and complex movement possibilities.

Thankfully, my stroke didn’t cause me to lose sensation in my arm and hand, and I love people touching my affected hand. When we had our first child, I came to realise that touch (including being touched) is “a basic behavioural need, much as breathing is a basic physical need”. Particularly when I couldn’t move my hand myself, I loved the sensation of someone else touching it (I still do). I found it reassuring and an intimate reaffirmation of a friendly/familial personal connection for someone to touch my non-moving hand and not be put off by it. The touch also sent sensory feedback to my brain, reminding me that my hand was still there, reminding me of how it could move.
I got a lot out of repeatedly following a couple of short Feldenkrais lessons for the hand by Annie Thoe, which really helped me to bring awareness to my hand once again. The videos were useful even when I couldn’t move my fingers unassisted. (I also loved that she says in one of them not to worry about not being able to move your hand after a stroke, adding “it’s going to wake up” — and since then it has for me!)
Moving a finger
I’m having a physio session. I look at my left hand and try to move a finger. I can’t. It’s like I don’t know how to any more. I stare at it again, and nothing happens. To get some idea of this, try to move one of your toes individually without moving any of the others (in bare feet). Most people find this incredibly hard and find it requires a lot of concentration.
The physio is great. He helps me to remember again how it feels to make the movement, by taking over and making the movement for me, with me. He tells me that the key here is my active involvement in the movement — to think about making the movement as he guides it, so that my brain is involved, even though I’m not yet able to make the move alone. This visualisation is a powerful (and tiring) technique. The physio then gets me to try again, alone.
The smaller the body part that you’re trying to move, the greater the intensity of concentration required. I stare at my finger; even a flicker of movement would be a great sign, because “wherever there is movement, however minute, there can be improvement.” Where there is no visible movement is where I need maximum concentration. As Tom Balchin explains, “even when there is literally no discernable movement, you are still stimulating neuroplastic change via the power of attention and visualisation alone.” This sort of visualisation is mentally tiring. After just a few minutes I’m sweating, and I’m exhausted by the end of the physio session. Not because my muscles are aching from a huge number of reps or from moving big weights, but because my brain is tired.
Mirror box therapy
I use a mirror box to help me with this mental exercise. I put my left hand behind a mirror and my right hand in front. I move my right hand and look at its reflection in the mirror.

The idea is to trick my brain into believing that the reflection of my right hand in the mirror is actually my left hand, and by looking at that to believe that I’m moving my left hand in the same way as my right hand. As I start to move my right hand, I am also exercising the part of my brain I need to move the other hand. Again, this is exhausting. After ten minutes my brain is tired.
The best bit about my rehab is when I find a virtuous circle. Once I’m able to move my arm a bit, it’s easier for me to remember to include it in my everyday activities. Using my arm enforces its place in my mental map of my body. Using it also reinforces the neural connections I’m using for that movement, and my muscles are no longer inactive and are exercising instead.
Small steps on my journey
I like to get a sense of me making progress in my recovery, and to help with that I keep a record of my physical rehab and of activities I can do again in everyday life. As my physical recovery has progressed, I have enjoyed a series of firsts, and in particular I enjoyed:
- the first time I could go to the toilet standing up
- the first time walking to the toilet by myself
- the first time I flushed the toilet with my left hand (both when I used a handle to do so and when I used a button)
- the first time getting in/out of the bath by myself
- the first time I had a shower by myself
- the first time I went for a walk out the house by myself
- the first time I could carry a tray
- the first time I could move and fill the kettle with my left hand
- the first time I opened a bottle of wine using both hands on a winged corkscrew
- the first time I made a hot drink in the morning and took it to Rebecca in bed
- the first time I could use our stove-top coffee pot, screwing it open and closed
- the first time we had sex again
- the first time holding a breadloaf in place as I cut it
- turning on/off a light switch
- pulling a light cord on/off
- opening/shutting a door with the handle
- the first time I chopped wood for kindling (even though I used the axe for this task one-handed with my right hand, it still felt like a step back towards normality)
- the first time I stacked logs
- the first time I could scratch an itch on my right arm with my left hand
- the first time I could do up the zip on my coat using my left hand
- the first time I tied my shoelace
- the first time I tied a double knot in my shoelace
- the first time reading a bedtime story with our two girls again
- the first time I used an exercise bike
- the first time I rode on a real bike again
- the first time I peeled and chopped cooking apples
- the first time I took a drink with my left hand (albeit with my right hand in a supporting role, which I still have to do)
- the first time carrying a bag in my left hand and not dropping it
- the first time being out by myself and getting taxi
- the first time going out to someone else’s house for a meal
- the first time going into a shop
- the first time going into a shop by myself
- the first time I didn’t go to bed at the same time as my girls but stayed up ‘late’ with Rebecca and watched a tv show
- my first time doing a chi gung form
- the first time I could hang from a bar and lift my feet off the ground (for 3 seconds)
- opening a tin of sardines (a two-handed job that I did for the first time this morning).
Where I am now
I’m very fortunate in that I’ve recovered almost all of my individual movement capabilities in my left arm. There are two main things that I’m aiming for now in my ongoing rehab and recovery.
First, I need to increase the strength in my arm, hand and fingers (both the strength of those muscles, and the strength of my neural connections for those muscles). Many of my movements are either slow or rather jerky. There are also many movements that I can do but cannot sustain or do consistently. One day I was putting some butter in our butter dish and trying to peel the wrapper off the butter with my left hand. I couldn’t pull it off, until with about my sixth attempt my grip on the wrapper was strong enough and it came off. One of my daughters said:
“it’s like you can only do it when you decide to do it.”
This is spot on. When I focus, I can get often get my arm/hand/fingers to do what I want. When I don’t, or when I stop, I can lose that control. I often drop things as they slip out of my hand. (As Rebecca points out this is partly a reflection of the fact that I’m doing more with my left hand. She’s right. But it’s still frustrating.) Things are harder when I’m tired, when I’m more likely to lose my concentration.
Second, I want to explore more complex movements and combinations of movements. Ahead of me, I see a number of steps still to come on my recovery journey:
- using a fork with my left hand so I can eat a meal with a knife and fork
- holding a book up to read with my left hand
- shuffling a pack of cards
- chopping wood using an axe with two hands
- carving a spoon
- going for a run
- driving a car
- swimming
- kayaking
And, thanks to the Feldenkrais method and continuum movement, I’m asking myself the question: what else is possible?
